How Long Does It Take For Dopamine Receptors To Recover From Addiction?
Dopamine receptors begin healing within 3 weeks of abstinence. Still, full recovery can take 3 to 12 months or longer, depending on factors such as the substance used, duration of addiction, and individual brain chemistry.

Dopamine receptors begin healing within 3 weeks of abstinence. Still, full recovery can take 3 to 12 months or longer, depending on factors such as the substance used, duration of addiction, and individual brain chemistry.
Dopamine receptor recovery isn't wishful thinking; it's a measurable neurological process with specific timelines, as supported by brain imaging studies.
Understanding these phases helps families set realistic expectations and recognize genuine progress during the challenging early recovery months.
Key Takeaways
-
Dopamine receptor recovery follows a predictable timeline: Recovery begins within weeks but requires 12-17 months for substantial restoration. Research shows dopamine transporter levels increase by 19% in the caudate and 16% in the putamen after 12-17 months of abstinence from methamphetamine. Complete normalization often takes 1-2+ years, with individual variation based on substance type and usage history.
-
Early recovery requires different family support than later stages: During the first 90 days, it takes about 90 days to notice a difference in experiences of pleasure and dopamine levels. The brain operates at severely reduced dopamine capacity, making it supportive in helping with daily tasks and decision-making. This compensates for temporary neurological deficits, not character flaws.
-
Progress markers appear at specific intervals: Initial recovery from cocaine exposure shows the first 15 days involve faster improvement (from >95% dysfunction to ~35%), but complete recovery takes about 60 days for single exposure. First mood improvements typically emerge around 30-90 days, with emotional stability returning between 3-6 months of sustained abstinence.
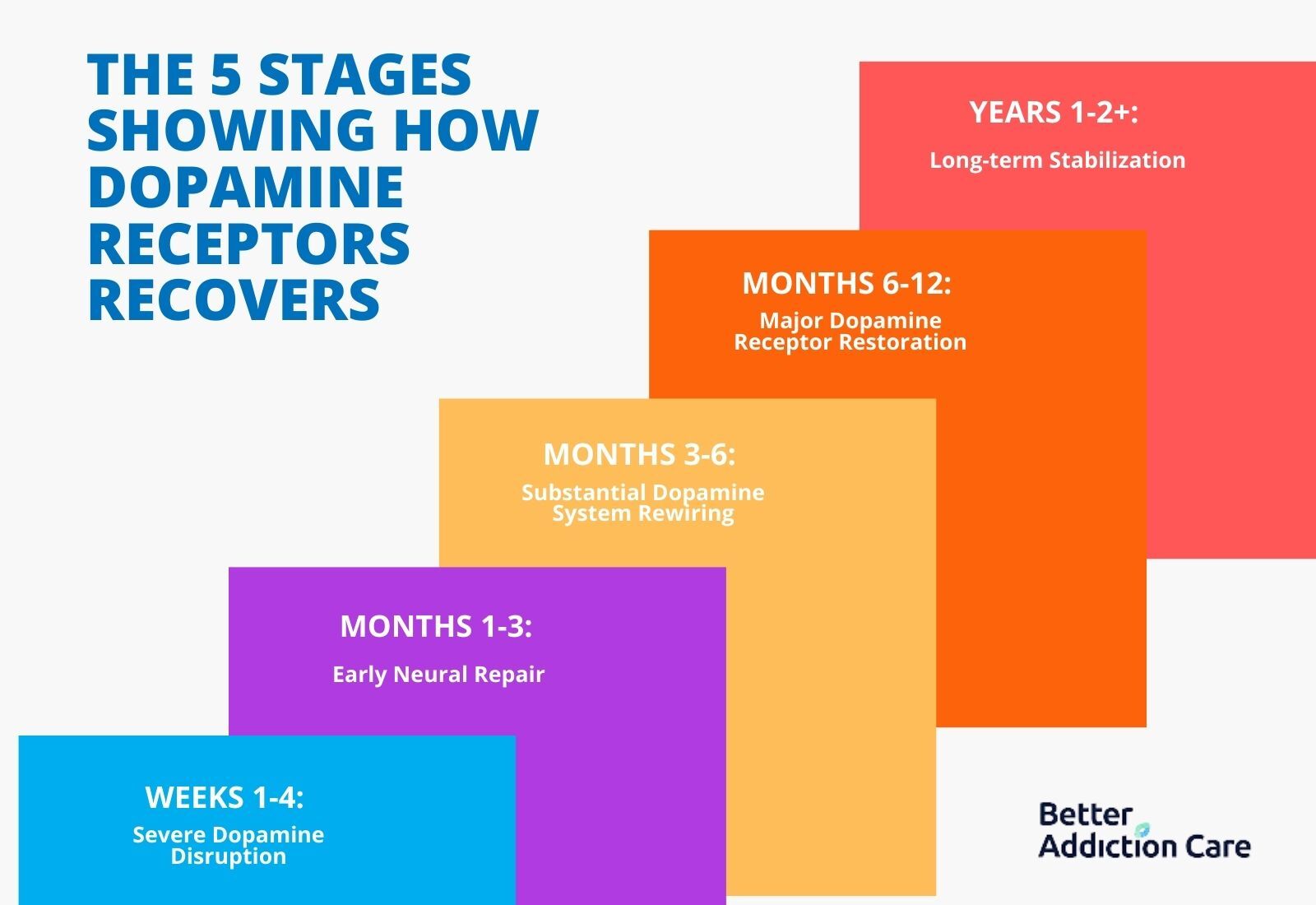
The 5 Stages below show how Recovery occurs for Dopamine Receptors.
-
Weeks 1-4: Severe Dopamine Disruption
-
Months 1-3: Early Neural Repair
-
Months 3-6: Substantial Dopamine System Rewiring
-
Months 6-12: Major Dopamine Receptor Restoration
-
Years 1-2+: Long-term Stabilization
Weeks 1-4: Severe Dopamine Disruption
The brain enters what researchers call a "hypodopaminergic state" during the first month of abstinence.
Chronic substance abuse results in the brain reducing the number of dopamine receptors or their sensitivity, meaning more of the substance or behavior is required to achieve the same pleasurable effect.
What's happening neurologically? Years of artificial dopamine flooding have caused receptors to downregulate (become less sensitive) and natural dopamine production to plummet.
The person experiences what addiction medicine calls "anhedonia", the inability to feel pleasure from normal activities.
Family reality check: If your loved one seems emotionally flat, struggles with basic decision-making, or shows little interest in activities they once enjoyed, this isn't laziness or lack of motivation. Their brain is operating with severely compromised reward circuits.
Communication approach: Keep interactions simple and concrete. Instead of "How are you feeling about recovery?" try "Have you eaten today?" or "Would you like to take a short walk?" Their cognitive processing is temporarily impaired, making complex emotional conversations difficult.
Months 1-3: Early Neural Repair
Research on cocaine recovery shows that after acute exposure, the initial recovery process from days 1 to 15 is relatively faster, but complete recovery of dopamine transporter distribution may take about 60 days. Studies show similar patterns across different substances.
Measurable improvements: Sleep patterns begin stabilizing, appetite returns more consistently, and brief moments of genuine pleasure become possible. However, many people describe "little moments" of normalcy during this period, but mood swings and cravings can still be intense.
Trust-building reality: This is when families often see improvement and assume "they're getting better," potentially leading to disappointment when setbacks occur. The brain is healing, but recovery is far from complete.
What helps: Celebrating small victories, enjoying a meal, laughing at a joke, or completing a simple task represents genuine neurological progress. Avoid the temptation to expect linear improvement.
Months 3-6: Substantial Dopamine System Rewiring
Animal studies show that D2 receptor availability following limited cocaine exposure in nonhuman primates recovered to control levels after only 1-3 months.
However, longer periods of exposure (12 months) showed recovery in only 60% of the subjects within 3 months.
Emotional regulation improvements: Many people experience steadier moods and increasing motivation during this period. The brain's stress response begins normalizing, reflected in a better ability to handle daily challenges and conflicts.
Communication breakthrough: Around month 4-6, families often notice their loved one becomes more emotionally available and capable of deeper conversations. This isn't coincidental; it reflects the prefrontal cortex regaining enough function to support complex emotional processing.
Relationship rebuilding: This is when trust conversations become more productive. The person can engage in planning, express genuine remorse, and follow through on commitments more consistently.

Months 6-12: Major Dopamine Receptor Restoration
After 14 months of abstinence, dopamine transporter levels (DAT) in the reward center of the brain are able to return to a nearly normal level of functioning. This represents the most significant phase of recovery for most people.
Personality changes: The person may report feeling more like their "old self," or even better. Simple pleasures register normally again, food tastes better, music is enjoyable, and social interactions feel rewarding rather than overwhelming.
Cognitive improvements: Memory, concentration, and decision-making abilities show substantial improvement. Many people return to work or school successfully during this period.
Family dynamics: Trust and communication often flourish around this time because genuine emotion and empathy flow again. However, some subtle vulnerability to stress may persist.
Years 1-2+: Long-term Stabilization
Brain imaging studies show that methamphetamine abusers evaluated during protracted abstinence (12-17 months) showed significant increases in dopamine transporters with 19% improvement in the caudate and 16% in the putamen. However, complete normalization continues beyond this point.
The new normal: Most people report permanent improvements by 2-3 years; they often feel not just like their old selves, but wiser and more emotionally mature. The brain has rewired itself differently than before addiction.
Ongoing neuroplasticity: Even after years, the brain continues adapting positively. People can continue strengthening healthy habits, and neuroplasticity remains active throughout life.
What are the Factors That Influence Dopamine Recovery Timeline?

Factors that influence dopamine recovery timeline include the type and duration of substance use, individual genetics, age, overall brain health, lifestyle choices, and the presence of supportive interventions like therapy, nutrition, and exercise.
1. Substance Type Creates
Stimulants (cocaine, methamphetamine): Complete recovery of dopamine transporter distribution may take about 60 days for a single stimulant like cocaine exposure, but with repeated exposures, recovery may take about 90 days. Heavy methamphetamine use often requires 12-18 months for substantial improvement.
Alcohol: Affects multiple neurotransmitter systems beyond dopamine. Brain volume recovery begins within 6-8 months, but emotional regulation may take 12-18 months to stabilize.
Opioids: Primarily suppress natural dopamine release rather than directly damaging receptors. Recovery patterns vary, but many people experience significant improvement within 6-12 months.
2. Duration and Intensity of Use
Methamphetamine abusers showed significant dopamine transporter reduction (27.8% in the caudate and 21.1% in the putamen) compared to controls, with this reduction evident even in abusers detoxified for at least 11 months. This demonstrates that heavier, longer-term use creates more extensive damage requiring longer recovery.
Daily vs. periodic use: Daily use creates deeper neural pathway changes than weekend or periodic use. The brain's reward circuits become more extensively rewired with consistent exposure.
Quantity consumed: Higher doses cause more severe receptor downregulation and require longer recovery periods. Each month of heavy use compounds the brain's structural changes.
3. Age at First Use
Adolescents who became abstinent from alcohol use showed significant recovery, but the developing brain is particularly vulnerable to addiction's rewiring effects.The prefrontal cortex doesn't fully mature until age 25, making teenage-onset addiction more complex to treat.
Adolescent-onset addiction: Usually requires 6-12 months longer for complete recovery compared to adult-onset addiction. The brain must both heal from addiction damage and complete normal development.
Adult-onset addiction: Generally follows more predictable recovery timelines, though individual variation remains significant.
4. Co-occurring Mental Health Conditions
Depression, anxiety, PTSD, or ADHD can extend dopamine recovery timelines:
-
Depression: Adds 6-9 months to emotional regulation recovery
-
Anxiety disorders: Delays stress response normalization by 3-6 months
-
ADHD: May slow prefrontal cortex healing by 4-8 months
-
Trauma/PTSD: Can extend overall recovery by 12-18 months
5. Physical Health and Lifestyle Factors
Accelerating factors:
-
Adequate sleep (7-9 hours nightly) supports neuroplasticity
-
Regular exercise increases BDNF (brain-derived neurotrophic factor) by up to 200%
-
Proper nutrition provides building blocks for neurotransmitter production
-
Stress management prevents cortisol from interfering with brain repair
Slowing factors:
-
Chronic sleep deprivation can slow neural recovery by 15-20%
-
Poor nutrition limits the brain's ability to rebuild neural pathways
-
Chronic stress floods the brain with cortisol, directly interfering with neuroplasticity
6. Support System Quality
Strong family support can accelerate recovery by 20-30%, while chaotic or enabling environments can extend timelines by 6-12 months. The emotional environment directly impacts stress hormones, which either support or hinder brain healing.
Supportive behaviors: Providing structure during early recovery, attending family therapy sessions, educating oneself about addiction as a brain disease, and maintaining healthy boundaries while showing love.
Enabling behaviors: Giving money without accountability, making excuses for harmful behavior, rescuing from natural consequences, or avoiding difficult conversations about recovery.
What are Strategies that Support Dopamine Recovery?
A. Medication-Assisted Treatment
With medication-assisted treatments, certain medications can support dopamine recovery:
Bupropion: An antidepressant that raises dopamine levels and can help reduce cravings and anhedonia during early recovery.
Modafinil: May be prescribed for daytime fatigue and concentration issues, particularly helpful during the 3-6 month period when cognitive function is still recovering.
Naltrexone: For alcohol use disorder, blocks opioid receptors and can help normalize dopamine function over time.
B. Behavioral Interventions
Cognitive Behavioral Therapy (CBT): Cognitive behavioral therapy is most effective once some dopamine function returns (after 3-6 months), as it requires cognitive processing abilities that are impaired in early recovery.
Contingency Management: Provides small, immediate rewards for abstinence, helping to retrain the brain's reward circuits during the vulnerable early recovery period.
Dialectical Behavior Therapy (DBT): Dialectical behavioral therapy is particularly effective during months 6-18 when emotional regulation is improving but still fragile.
C. Lifestyle Interventions
Structured exercise: The brain naturally releases dopamine when you exercise. Even 30 minutes of moderate exercise 3-4 times weekly can significantly support dopamine recovery.
Mindfulness practices: Meditation, yoga, and deep breathing exercises help manage stress and support neuroplasticity without overwhelming the recovering brain.
Social connection: Healthy relationships provide natural dopamine release and support emotional regulation during recovery.
Sleep hygiene: The brain does much of its repair during deep sleep phases. Consistent sleep schedules and good sleep hygiene are crucial for optimal recovery.
When to Seek Professional Help during Dopamine Receptor Recovery?
When symptoms like persistent depression, extreme mood swings, or inability to feel pleasure continue beyond a few weeks of recovery, it's important to consult a mental health professional.
Early intervention from professional addiction specialists helps tailor treatment strategies and prevent long-term neurological or emotional complications by addressing underlying behavioral patterns, restoring dopamine balance, and promoting healthier coping mechanisms for sustained recovery.
-
Severe depression or suicidal thoughts
-
Inability to sleep or eat for several days
-
Extreme agitation or psychosis
-
Medical complications from withdrawal
-
Inability to function in daily life despite sobriety
-
Continued cognitive impairment interfering with work or relationships
-
New addictive behaviors emerging
-
Regression in emotional or cognitive function
-
Persistent relationship difficulties despite sobriety
-
Ongoing inability to experience pleasure from any activities
-
Increased risk-taking or impulsive behaviors
Frequently Asked Questions
Listed below are frequently asked questions about Dopamine receptor recovery.
How long does it really take for dopamine receptors to recover?
Research shows substantial recovery occurs within 12-17 months, with dopamine transporter levels increasing by 19% in the caudate and 16% in the putamen during this period. However, complete normalization often takes 1-2+ years, depending on substance type, duration of use, and individual factors.
Can brain scans show dopamine recovery?
Yes, brain imaging studies can measure dopamine transporter density and receptor availability throughout recovery. PET scans show that after 14 months of abstinence, dopamine transporter levels in the reward center return to nearly normal functioning. These scans provide concrete evidence of healing progress.
What if there's a relapse during recovery?
Research shows that even after relapse, the brain retains some capacity for recovery, though repeated exposure can slow the process. Each recovery period allows some neural healing to occur, often making subsequent recovery efforts more successful. Relapse doesn't erase all progress, it's a sign that additional support and structure are needed.
Are there genetic factors affecting recovery speed?
Yes, genetic variations in dopamine receptors and transporters can influence recovery speed. Family history of addiction often correlates with 10-15% longer recovery times. However, genetic predisposition doesn't prevent recovery, it simply means the timeline may be extended and more support may be needed.
Can dopamine receptors fully heal from addiction?
In general, it takes the brain up to 14 months to recover, with brain scans showing significant improvement in just one month of abstinence. While some structural changes may be permanent, the brain's neuroplasticity allows it to develop new pathways and adapt effectively. Many people report their post-recovery brain function is actually better than before addiction.
Conclusion:
Dopamine receptor recovery is neither quick nor simple, but it is profoundly hopeful.
Research definitively shows that protracted abstinence can reverse methamphetamine-induced alterations in brain dopamine terminals.
The human brain's capacity for healing, neuroplasticity, offers genuine hope for recovery.
The timeline requires patience: weeks for stabilization, months for substantial improvement, and years for complete normalization. But each phase brings measurable progress. The first genuine laugh, the return of appetite, the ability to concentrate on a task, these represent real neurological healing.
Families play a crucial role in this process. Understanding that early recovery involves compensating for temporary brain deficits, not enabling destructive choices, helps provide appropriate support. Recognizing that emotional availability and trust-building capacity follow predictable timelines prevents unrealistic expectations and disappointment.
The recovery journey transforms not just the individual but often the entire family system. As one family member shared: "Recovery isn't about getting the old person back, it's about building a relationship with who they're becoming. Their brain is literally different now, and in many ways, that's been a gift."
With proper support, medical care, and realistic expectations, dopamine receptor recovery offers the foundation for a life that's not just free from addiction, but often richer and more meaningful than before.
Resources
-
Journal of Neuroscience"Loss of dopamine transporters in methamphetamine abusers recovers with protracted abstinence."Retrieved on July 17, 2025
-
American Journal of Psychiatry,"Association of dopamine transporter reduction with psychomotor impairment in methamphetamine abusers."Retrieved on July 22, 2025
-
Journal of Biological Chemistry"Recovery of dopaminergic system after cocaine exposure and impact of a long-acting cocaine hydrolase."Retrieved on July 22, 2025
-
Neuropsychopharmacology"Recovering from Cocaine: Insights from Clinical and Preclinical Investigations"Retrieved on July 22, 2025
-
NPR Life Kit"Break the cycle of addiction with these strategies to keep dopamine in check"Retrieved on July 22, 2025
Related Articles
Treatment Centers in New York







