What is a Relapse? Warning Signs, Triggers, & Treatment
A relapse is the return of addiction, illness or problematic behaviors after a period of recovery, indicating a setback in an individual's condition, often seen in chronic diseases, addiction, or psychiatric disorders.

A relapse is the return of addiction, illness or problematic behaviors after a period of recovery, indicating a setback in an individual's condition, often seen in chronic diseases, addiction, or psychiatric disorders.
According to Mao, S. 's 2024 study, ‘A probabilistic model of relapse in drug addiction.’, more than 60% of individuals recovering from substance use disorder relapse within one year, as reported by the National Institute of Drug Abuse (NIDA). The data shows that relapse risk is highest during the first months after detoxification, though relapse remains possible even after many years of abstinence. Specifically for opioid abuse disorder patients, studies indicate relapse rates of approximately 40 to 60 percent one year after treatment.
Warning signs of a relapse include mood changes such as irritability and anxiety, behavioral shifts like isolation and neglect of responsibilities, intense cravings for substances, denial of addiction severity, neglect of recovery practices, social withdrawal from supportive networks, cognitive issues like poor concentration, physical changes in sleep and hygiene, and exposure to triggers associated with past substance use.
Common triggers for alcohol and drug relapse include exposure to intoxicating substances, high-stress situations, drug paraphernalia, and environments or social circles linked to past substance use, highlighting the importance of recognizing these factors to develop effective relapse prevention strategies in recovery.
Treatment options for relapse on drugs or alcohol include Medication-Assisted Therapy (MAT) to reduce cravings, Cognitive Behavioral Therapy (CBT) for trigger management, support systems like 12-step programs, Intensive Outpatient Programs (IOP) for structured therapy, holistic approaches such as mindfulness, and continued care through long-term outpatient programs.
What is a Relapse?
A relapse is the recurrence of illness, addiction, symptoms, or problematic behaviors after a period of improvement or recovery. It represents a deterioration in a person's condition, typically occurring in chronic diseases, addiction disorders, or psychiatric conditions where the individual returns to previous patterns of dysfunction despite having shown progress toward health or sobriety.
Is a Slip the Same as a Relapse?
No, a slip and a relapse are not exactly the same, though they are closely related. A slip typically refers to a single, accidental instance of substance use during recovery, such as an alcoholic having one drink at a social event. In contrast, a relapse generally indicates a more significant return to substance use patterns where the person has abandoned their recovery plan altogether.
The key difference lies in the recovering person's intentions and response. A slip is characterized by unplanned use followed by immediate efforts to get back on track—like attending a meeting or consulting a therapist. A relapse, however, involves a conscious decision to resume using substances without taking steps to return to sobriety. A slip leads to a relapse, but it is not inevitable if the person quickly recommits to their recovery and seeks the right support.
What Are The Stages of Relapse?
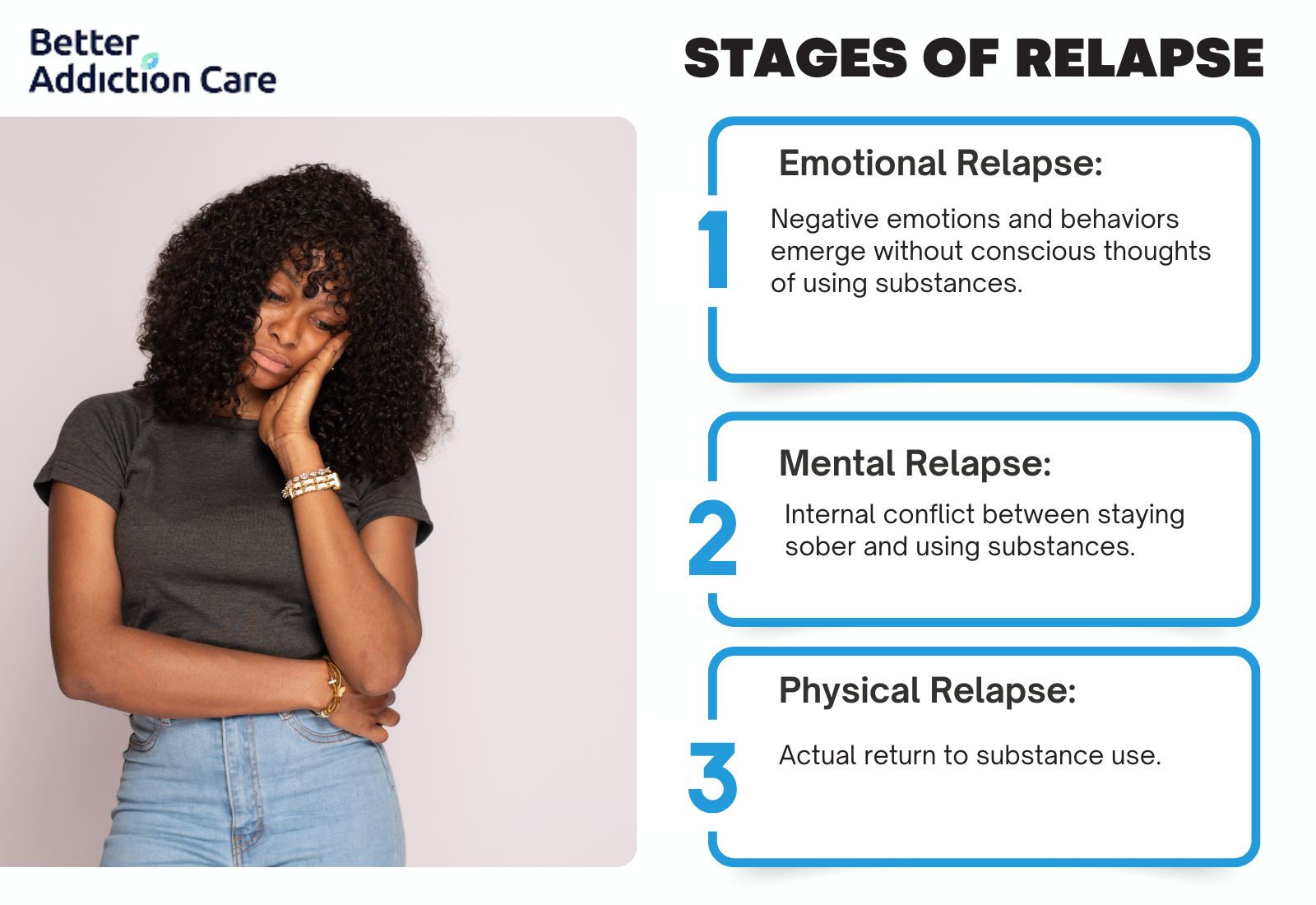
The stages of relapse include emotional, mental, and physical phases that represent a progressive path toward potential substance use. Emotional relapse begins with negative emotions and self-care neglect, mental relapse involves internal struggles with cravings and substance-related thoughts, while physical relapse occurs when actual substance use takes place.
Here are the stages of relapse in detail below:
Stage 1: Emotional Relapse: During emotional relapse, individuals experience negative emotions and behaviors without consciously considering substance use. Signs include:
-
Poor eating and sleeping habits
-
Isolation from support networks
-
Skipping recovery meetings or not participating
-
Neglecting self-care routines
-
Abandoning recovery practices like the 12 steps
-
Focusing excessively on others' problems
This stage involves denial about relapse risk, making recognition difficult. Intervention focuses on emphasizing self-care practices and acknowledging denial patterns.
Stage 2: Mental Relapse: Mental relapse involves an internal struggle between sobriety maintenance and substance use desires. Indicators include:
-
Experiencing intense cravings
-
Reminiscing about past substance use
-
Bargaining about controlled usage
-
Dishonesty with self and others
-
Seeking opportunities to use substances
-
Planning relapse scenarios
-
Associating with people and places from past usage
This phase requires active avoidance of high-risk situations, increased participation in support meetings, and reinforcement of sobriety benefits through connections with sober individuals.
Stage 3: Physical Relapse: Physical relapse occurs when an individual returns to actual substance use. This represents the culmination of the emotional and mental stages. Recovery from physical relapse necessitates immediate reengagement with treatment programs to reestablish sobriety and strengthen prevention strategies.
Recognition of early relapse warning signs allows for intervention before physical relapse occurs. Recovery involves understanding that relapses indicate a need for treatment adjustment rather than representing personal failure. Success in recovery comes through continuous vigilance, support utilization, and adaptive coping skill development.
What Are The Warning Signs Of A Relapse?

The Warning Signs Of A Relapse include mood swings, behavioral changes, intense cravings, denial patterns, abandoning recovery activities, isolation from supporters, cognitive dysfunction, physical health deterioration, and trigger exposure.
Here are the warning signs of a relapse in detail below:
-
Mood Changes: Increased irritability, depression, or anxiety signal emotional distress, often linked to relapse triggers.
-
Behavioral Shifts: Isolation, secrecy, or neglecting responsibilities (e.g., skipping work or family obligations) indicate potential regression.
-
Cravings: Intense urges to reuse substances or engage in addictive behaviors, often accompanied by fantasizing about past use.
-
Denial or Minimization: Downplaying the severity of addiction or dismissing recovery efforts, such as justifying occasional use.
-
Neglecting Recovery Practices: Stopping therapy, skipping support group meetings, or discontinuing prescribed medication.
-
Social Withdrawal: Avoiding contact with a support network, sponsors, or friends who encourage sobriety.
-
Cognitive Issues: Poor concentration, memory lapses, or mental fog, which precede impulsive decisions.
-
Physical Signs: Changes in sleep patterns, appetite, or personal hygiene, often reflecting emotional turmoil.
-
Exposure to Triggers: Re-engaging with high-risk environments, stress, or conflicts linked to past substance use.
What Are The Alcohol And Drug Relapse Triggers?

The alcohol and drug relapse triggers include encountering intoxicating substances, experiencing high stress situations, seeing drug paraphernalia, and revisiting locations or social circles connected to past substance use. Understanding these common triggers is essential for developing effective relapse prevention strategies in recovery.
According to Nguyen, L. C.’s 2020 study, ‘Predicting relapse after alcohol use disorder treatment in a high-risk cohort: The roles of anhedonia and smoking.’, on predicting relapse after alcohol use disorder (AUD) treatment, approximately 69% of Veterans relapsed within six months of completing treatment, while only 31% maintained abstinence. This aligns with general statistics showing that about two-thirds of individuals treated for AUD relapse within six months. The study identified several significant predictors of relapse, including higher levels of anhedonia (loss of pleasure), active smoking status, and fewer days of abstinence prior to treatment.
Here are the common alcohol and drug release triggers:
-
Alcohol consumption: Alcohol heightens the temptation to use drugs of abuse. As a depressant, alcohol has a strong effect on the brain when combined with other substances. If a person with a substance use disorder begins to drink, it intensifies their desire to use other substances.
-
Stress: Stress functions as a significant trigger for people recovering from substance use disorder. When someone experiences significant stress, they need healthy coping mechanisms rather than returning to substance use.
-
Paraphernalia: The equipment people use to consume their substance of choice. People in recovery must keep paraphernalia out of sight and avoid situations where others are using.
-
People/Places: Environmental factors trigger urges to use. Being around people, places, and situations associated with past substance use increases relapse likelihood.
What Are The Treatment Options For A Relapse On Drugs Or Alcohol?

The treatment options for a relapse on drugs or alcohol include Medication-Assisted Therapy with FDA-approved medications to reduce cravings, Cognitive Behavioral Therapy to identify triggers, support systems like 12-step programs, Intensive Outpatient Programs that balance recovery with daily life, holistic approaches such as mindfulness practices, and continued care through long-term outpatient programs.
Here are the key treatment options for a relapse on drugs or alcohol:
Medication-Assisted Therapy (MAT)
Medication-Assisted Therapy (MAT) uses FDA-approved medications like disulfiram, acamprosate, and naltrexone to reduce cravings and block the euphoric effects of alcohol. For opioid relapse, medications such as methadone, buprenorphine, and naltrexone stabilize brain chemistry and prevent withdrawal. Regular medical monitoring ensures adherence and adjusts dosages to manage side effects.
Effective recovery programs incorporate Medication-Assisted Therapy (MAT) with counseling and behavioral therapies for a complete treatment approach. This combination addresses both physical dependence and psychological addiction patterns, resulting in higher success rates and fewer instances of relapse.
Cognitive Behavioral Therapy (CBT)
CBT helps identify triggers and develop coping strategies to avoid relapse. Techniques such as contingency management (which uses rewards to incentivize sobriety) are often integrated into CBT frameworks, enhancing effectiveness for stimulant and opioid use disorders. Therapy sessions emphasize skill-building, including stress management and refusal techniques. CBT also addresses negative thought patterns linked to addiction, reducing the risk of future relapse.
Support Systems
12-step programs (e.g., Alcoholics Anonymous) provide peer-led accountability and structured recovery steps. Support groups (e.g., SMART Recovery) offer non-spiritual, science-based tools for relapse prevention. Engaging with sponsors or peer networks reinforces commitment to sobriety.
Intensive Outpatient Programs (IOP)
IOPs provide structured therapy sessions (e.g., 9–12 hours per week) while allowing patients to live at home, balancing recovery with daily responsibilities. These IOP programs combine group therapy, individual counseling, and relapse prevention planning, often incorporating CBT principles. IOPs are ideal for individuals transitioning from inpatient care or those needing more support than standard outpatient services.
Holistic Approaches
Mindfulness practices and stress-reduction techniques (e.g., biofeedback) help manage cravings by regulating emotional responses. Nutritional counseling and exercise improve physical health, which often deteriorates during relapse.
Continued Care
Long-term outpatient programs and aftercare plans sustain recovery through regular therapy sessions, medication management, and check-ins. Ongoing monitoring via urine tests or digital tools (e.g., apps) tracks progress and flags risks.
What to Do if You Are Experiencing Relapse Triggers?
If you are experiencing relapse triggers, identifying them is crucial for supporting yourself or loved ones in recovery. Seek support through individual therapy, group therapy, or support groups such as AA, NA, or SMART Recovery. The more support received, the better the chances of avoiding a potential relapse. Additionally, revisit coping skills, which include exercising, meditation, positive reframing, spiritual practices, art therapy, writing or journaling, and volunteering.
What Are the Key Elements of Effective Relapse Prevention?
The key elements of effective relapse prevention are understanding recovery stages, managing withdrawal, following fundamental rules, utilizing cognitive therapy, and recognizing relapse opportunities.
According to Melemis SM.’s 2015 study, ‘Relapse Prevention and the Five Rules of Recovery.’, recovery progresses through three distinct stages with unique relapse risks: the abstinence stage lasting 1-2 years, the repair stage lasting 2-3 years, and the growth stage. Post-acute withdrawal syndrome persists up to 2 years with varying symptoms. Recovery success depends on five essential rules: changing your life to create an environment where abstinence comes easier, maintaining complete honesty, asking for help when needed, practicing consistent self-care, and following recovery guidelines without exception. Cognitive therapy demonstrates effectiveness for relapse prevention in numerous studies. Physical relapses typically occur as "relapses of opportunity" when individuals believe they avoid detection.
How to Connect with Relapse Recovery Treatment Programs Near You?
Connecting with the right treatment program after experiencing a relapse starts with reaching out for professional guidance. Call our 24/7 confidential helpline at (800) 429-7690. Speak with addiction specialists. Specialists match you with rehab centers in your area. Verify your insurance coverage online. Understand your financial options. Explore local treatment centers in California, Florida, or Massachusetts. Determine whether inpatient detox, outpatient rehabilitation, or support groups address your specific needs. Remember that seeking help after a relapse isn't a sign of failure, but rather an important step in your ongoing recovery journey that will help reinforce your relapse prevention skills and coping strategies.
Related Articles
Treatment Centers in Georgia







