Different Levels of Care for Treating Addiction

Levels of Care in Addiction Treatment is a structured continuum of services aimed at addressing the diverse needs of individuals with substance use disorders, ranging from least to most intensive based on the severity of addiction and personal circumstances. The American Society of Addiction Medicine (ASAM) plays a vital role in this framework by evaluating various dimensions, including medical, psychiatric, and environmental factors, to determine the most suitable level of care for effective treatment and recovery.
ASAM's Five Levels of Care Programs provide a comprehensive continuum of addiction treatment services, from early intervention (Level 0.5) to medically managed intensive inpatient services (Level 4), matching individuals with appropriate care based on their needs and the severity of their substance use disorder. Each level offers tailored interventions, including prevention strategies, outpatient services, intensive outpatient care, residential treatment, and hospital-based programs, emphasizing effective, evidence-based treatment options for successful recovery outcomes.
The range of costs of different levels of care in addiction treatment varies significantly. Outpatient services cost $100 to $500 per session, while intensive outpatient programs range from $300 to $1,000 weekly. Residential care costs between $200 and $1,000 daily, depending on intensity, and medically managed inpatient services range from $1,000 to $2,000 daily. Low-intensity residential services start at $200 per day, while high-intensity options average $184 to $400 per day. Medically monitored inpatient and detoxification services represent the highest costs, reflecting the comprehensive care needed for severe addiction cases.
According to Barocas, J.A.’s 2022 study, ‘Clinical impact, costs, and cost-effectiveness of hospital-based strategies for addressing the US opioid epidemic: a modelling study, ’ addiction treatment costs vary significantly across different hospital-based intervention strategies. The research identified mean lifetime costs of US$731,400 (95% credible interval 447,911–859,189) for the medications for opioid use disorder strategy and $741,200 (470,930–868,551) for the combined strategy per person. The cost-effectiveness analysis determined that medications for opioid use disorder with bridge prescriptions cost $7,600 per life-year gained, while the combined approach of expanded medications with addiction consult services cost $14,300 per life-year gained. Both strategies fell well below the $100,000 per life-year gained threshold, confirming their cost-effectiveness in addressing the US opioid epidemic.
What Are the Levels of Care in Addiction Treatment?
Levels of Care in Addiction Treatment refer to a structured continuum of services designed to address the varying needs of individuals with substance use disorders. These levels range from least to most intensive and are tailored based on the severity of the addiction, the individual's living situation, and their progress in recovery.
What Is ASAM, and What Are Its Dimensions?
ASAM (American Society of Addiction Medicine) is a professional medical society dedicated to increasing access to and improving the quality of addiction treatment, educating physicians and other healthcare providers, and advocating for public policy that promotes addiction prevention and treatment. Founded in 1954, ASAM represents over 7,000 physicians, clinicians, and other professionals who specialize in addiction medicine, providing evidence-based guidelines, educational resources, and certification programs for the diagnosis and treatment of addiction and substance use disorders.
ASAM evaluates different dimensions to determine the right level of care. These dimensions are:
-
Dimension 1 - Intoxication, Withdrawal, and Addiction Medications: Assesses acute intoxication and associated risks, withdrawal and associated risks, and addiction medication needs.
-
Dimension 2 - Biomedical Conditions: Evaluates physical health concerns, pregnancy-related concerns, and sleep problems.
-
Dimension 3 - Psychiatric and Cognitive Conditions: Examines active psychiatric concerns, persistent disability, cognitive functioning, trauma exposure and related needs, and psychiatric and cognitive history.
-
Dimension 4 - Substance Use Related Risks: Assesses likelihood of risky substance use and likelihood of risky SUD-related behaviors.
-
Dimension 5 - Recovery Environment Interactions: Evaluates the ability to function in the current environment, safety in the current environment, support in the current environment, and cultural perceptions of substance use.
-
Dimension 6 - Person-Centered Considerations: Addresses patient preferences, barriers to care, and need for motivational enhancement.
What Are ASAM's Five Levels of Care Programs?

ASAM's Five Levels of Care Programs are a comprehensive continuum of addiction treatment services ranging from early intervention (Level 0.5) to outpatient services (Level 1), intensive outpatient/partial hospitalization (Level 2), residential/inpatient treatment (Level 3), and medically managed intensive inpatient services (Level 4), designed to match individuals with the appropriate level of care based on their specific needs and the severity of their substance use disorder.
Here are the five levels of care programs in detail below:
Level .5 Prevention/Early Intervention:
Level 0.5 – Early Intervention is a preventive program that provides education and brief counseling to individuals at risk for substance misuse, offering risk-reduction strategies and community outreach to prevent progression to more severe use. This level is designed for individuals who do not meet the criteria for substance use disorder but are at risk.
Services include:
-
One-on-one counseling: One-on-one counseling is a personalized service that provides individual therapy to address behavioral health and substance use challenges.
-
Drug-free workplace initiatives: Drug-free workplace initiatives are programs designed to maintain a safe and healthy work environment by preventing substance misuse and promoting employee wellness.
-
SBIRT: Screening, Brief Intervention, and Referral to Treatment: SBIRT (Screening, Brief Intervention, and Referral to Treatment) is an approach that identifies at-risk individuals, provides immediate intervention, and connects them to specialized treatment.
-
Employee Assistance Programs: Employee Assistance Programs are employer-sponsored services that offer confidential counseling and support for personal and work-related issues.
Level 1. Outpatient Services:
Level 1 – Outpatient Services are treatment programs delivered in a non-residential setting that allow individuals to attend scheduled therapy sessions while continuing their daily activities, with clinical contact under nine hours per week. Provides services for individuals with mild or moderate substance use disorders.
According to Molfenter T. D.’s 2014 study, ‘Addiction treatment centers' progress in preparing for health care reform, ’ outpatient services were the most commonly provided level of care among addiction treatment organizations, with 88% of the surveyed 427 organizations offering these services. This was higher than the national average of 81% reported in the SAMHSA 2011 National Survey of Substance Abuse Treatment Services.
Services could include:
-
Psychotherapy for individuals and groups: A service that provides structured therapeutic sessions for individuals or groups to address mental health issues and promote behavioral change.
-
Psychoeducational services: Programs that deliver information and skills training to enhance clients' understanding of their conditions and foster effective self-management.
-
Family and adjunctive therapies: Therapeutic interventions that involve family members and support networks to improve communication, resolve conflicts, and strengthen the overall treatment process.
-
Nursing services: Professional healthcare support that offers medical assessment, ongoing monitoring, and care coordination to ensure patient safety and comfort.
-
Ambulatory services: Outpatient care that delivers medical, therapeutic, or diagnostic services without requiring an overnight stay in a facility.
-
Medication Management: A process that oversees the prescription, administration, and monitoring of medications to optimize treatment outcomes.
-
Medicated Assisted Treatment: A service that integrates the use of medications with counseling and behavioral therapies to treat substance use disorders.
-
Laboratory/Toxicology Services: Diagnostic testing procedures that assess biological samples to monitor treatment progress and detect the presence of substances.
Level 2. Crisis Stabilization/ Intensive Outpatient:
Level 2 covers services that address the unique needs of individuals with addiction and any other type of co-occurring conditions. It is structured as an outpatient program in which treatment services are provided during the day.
Level 2.1 Intensive Outpatient Services
Level 2.1 is known as a Referred Intensive Outpatient Treatment for Adolescents and Adults. This level of care is defined as administering at least 9 to 19 hours per week for adults and at least 6 hours for adolescents. The key is that care is provided while treating multidimensional instability.
Level 2.5 Partial Hospitalization Services
Offering 20 or more hours of treatment per week, this sublevel provides comprehensive services for individuals needing substantial support without full hospitalization.
Level 2.7 Medically Managed Intensive Outpatients
Based on medically managed intensive outpatient therapy that does not need 24-hour monitoring.
Level 3. Residential/Inpatient Services:
Level 3 – Residential/Inpatient Services are 24-hour structured treatment programs provided in a live-in facility, offering a range of services from low-intensity supportive living to high-intensity therapeutic interventions and medically monitored care for complex cases.
According to Molfenter T. D.’s 2014 study, ‘Addiction treatment centers' progress in preparing for health care reform, ’ residential treatment services were provided by 46% of the surveyed addiction treatment organizations, which was significantly higher than the national average of 32%. This suggests that the organizations participating in the Health Reform Readiness Index survey were more likely to offer residential care compared to the national sample.
Level 3.1 Clinically Managed Low-Intensity Residential Services:
Treatment programs in this category include a variety of therapeutic interventions, for instance, individual and group psychotherapy, psychoeducational services, family and adjunctive therapies, nursing services, medication management, medication-assisted treatment, laboratory/toxicology services, and housing and community resource building.
Level 3.5 Clinically Managed High-Intensity Residential Services:
This level of care is called Clinically Managed Medium-Intensity Residential Services for adolescents and Clinically Managed High-Intensity Residential Services for adults, and it provides 24-hour medical care and support from trained counselors.
This aims to stabilize people threatened by multidimensional imminent danger and prepare them for outpatient care. The expansive services offered include individual and group psychotherapy, psychoeducational services, family and adjunctive therapies, nursing services, medication management, and help with housing and community resources.
Level 3.7 Medically Monitored High-Intensity Inpatient Services:
This type of care is called Medically Monitored High-Intensity Inpatient Services for adolescents and Medically Monitored Intensive Inpatient Services Withdrawal Management for adults, and it offers 24/7 nursing monitoring with physicians available to address significant issues in Dimensions 1, 2, or 3.
It provides the right environment for patients with subacute biomedical and psycho-behavioral or psycho-cognitive challenges that are severe enough to require inpatient care.
Services rendered are a multitude of interventions and include individual and group psychotherapy, psychoeducational services, family and adjunctive therapies, nursing services, medication management, medication-assisted treatment, and laboratory/toxicology services.
Level 4. Medically Managed Intensive Inpatient Services:
Level 4 – Medically Managed Intensive Inpatient Services are hospital-based programs that provide full 24-hour medical and nursing care for individuals with severe substance use disorders and associated medical complications.
Level 4 programs are staffed with a team of licensed and certified professionals who provide continuous medical management by physicians, primary nursing care, observation, and professional counseling services for 16 hours daily.
Transition from one of these numbered levels to another is possible, and referral is possible in the upper or lower direction as required and determined by the specialist. This systematic model emphasizes ASAM's dedication to offering personalized treatment programs to help patients in their recovery process.
What Are the Costs of Different Levels of Care in Addiction Treatment?
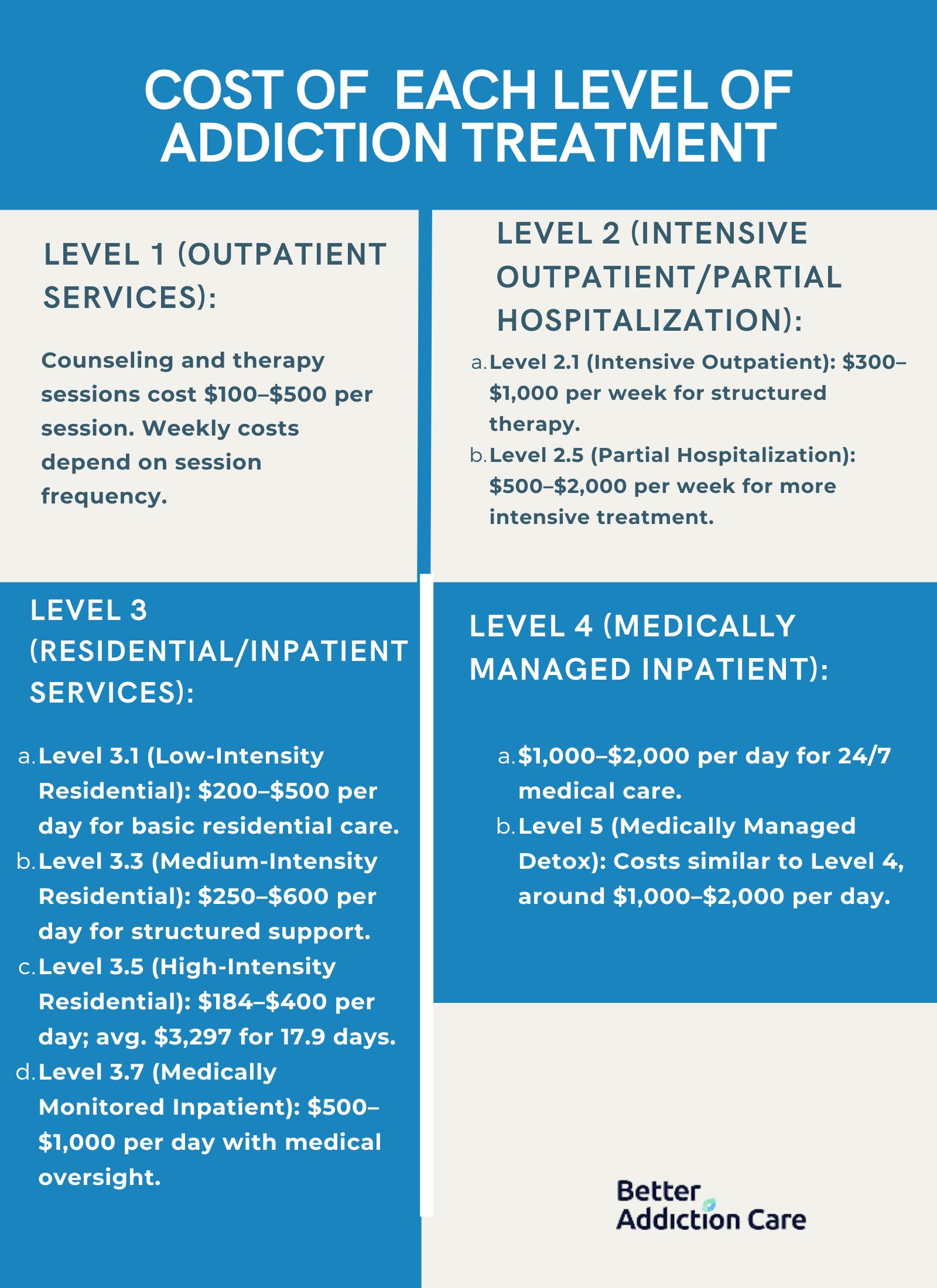
The costs of different levels of care in addiction treatment include outpatient services ranging from $100-500 per session, intensive outpatient programs at $300-1,000 weekly, residential care varying from $200-1,000 daily depending on intensity, and medically managed inpatient services costing $1,000-2,000 daily.
Here are the costs of different services in levels of care in addiction treatment in detail below:
-
Level 1: Outpatient Services: Outpatient services include individual counseling, group therapy, and educational sessions. These services cost between $100 and $500 per session. Weekly costs vary based on the frequency of sessions.
-
Level 2: Intensive Outpatient/Partial Hospitalization Services:
-
Level 2.1 (Intensive Outpatient): Intensive outpatient programs provide structured therapy sessions several times a week. Costs range from $300 to $1,000 per week.
-
Level 2.5 (Partial Hospitalization): Partial hospitalization programs offer more extensive treatment hours, including therapy and medical monitoring. Costs are between $500 and $2,000 per week.
-
Level 3: Residential/Inpatient Services:
-
Level 3.1 (Clinically Managed Low-Intensity Residential Services): These services include basic residential care with minimal medical oversight. Costs are between $200 and $500 per day.
-
Level 3.3 (Clinically Managed Medium-Intensity Residential Services): Medium-intensity residential services provide more structured therapy and support. Costs range from $250 to $600 per day.
-
Level 3.5 (Clinically Managed High-Intensity Residential Services): High-intensity residential services offer intensive therapy and support. The average total cost for a stay is about $3,297 for 17.9 days, which translates to approximately $184 to $400 per day.
-
Level 3.7 (Medically Monitored High-Intensity Inpatient Services): These services include medical monitoring and intensive therapy. Costs are between $500 and $1,000 per day.
-
Level 4: Medically Managed Intensive Inpatient Services: Medically managed intensive inpatient services include 24-hour medical care, intensive therapy, and medication management. Costs range from $1,000 to $2,000 per day.
-
Level 5: Medically Managed Detoxification Services: Medically managed detoxification services provide intensive medical supervision during withdrawal. Costs are generally similar to Level 4 services, often between $1,000 and $2,000 per day.
Why Is It Necessary to Have Different Levels of Care?
Different levels of care are necessary because no single treatment approach is effective for everyone. Individuals present with unique combinations of physical, psychological, and medical conditions, as well as varying degrees of social support and personal circumstances that must be considered when determining appropriate therapy.
Effective treatment requires a comprehensive, individualized approach tailored to each person's specific condition or conditions. This personalization is essential for successful outcomes.
The American Society of Addiction Medicine (ASAM) has established systematic criteria to guide decisions about placement, continuation, transfer, or discharge from treatment. Many treatment centers implement these guidelines to provide distinct levels of care, ensuring patients receive treatment that aligns with their specific needs and significantly improving their chances of successful recovery.
Where to Find the Rehab Center for the Right Level of Care for Me?
Finding the right level of care for yourself starts with professional guidance. You don't have to navigate this journey alone—doctors and addiction specialists help determine your appropriate treatment needs. These healthcare professionals are trained to assess your specific situation and recommend personalized care options that address your unique circumstances and recovery goals.
The recovery process begins with a series of tasks to determine the best initial treatment and set the path for a process that will indeed have a multitude of evaluations and assessments during its length. Finding the proper assistance and tools means you will make your journey to recovery with the aid of a talented counselor. You use our Treatment Centers Finder to get information about the nearest place where you go for assistance.





